In Northern Ireland, around 1200 men and women are diagnosed with bowel cancer every year. It is one of the most common causes of cancer deaths with about 450 deaths each year. However, if diagnosed early, bowel cancer is highly treatable.
The Bowel
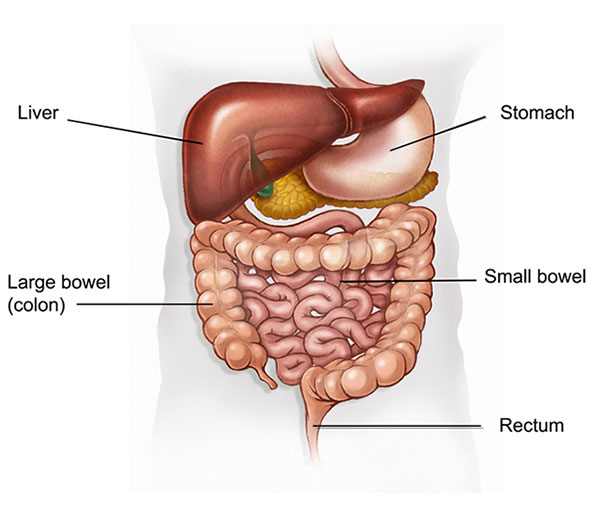
The bowel is part of the digestive system and is divided into the small bowel (small intestine) and the large bowel (colon and rectum). As digested food leaves the small bowel it enters the large bowel where water and salts are absorbed. The muscles of the large bowel move the waste towards the rectum and anus where it leaves the body.
 Risk factors of bowel cancer
Risk factors of bowel cancer
Age:
Bowel cancer risk increases with age. Around 93% of cases occur in people over the age 50 but it can still develop in younger people.
Family history of bowel cancer:
If one or more close relatives (parent, brother or sister) have been diagnosed with bowel cancer before the age of 45, there is a possibility the condition is hereditary.
Other bowel conditions:
Long-standing inflammatory diseases of the bowel such as Crohn’s disease or ulcerative colitis may increase the risk of bowel cancer. Bowel polyps (growths) could potentially become cancerous if left untreated and allowed to grow beyond a certain size.
Diabetes:
There is an increased risk of developing bowel cancer if you have diabetes. However, the reason is not clear. Research is currently being carried out in this area.
Symptoms of bowel cancer
- Bleeding from the rectum (back passage) and/or blood in your bowel movement lasting 2-3 weeks
- A change in bowel habit lasting 6 weeks or more (e.g. more frequent or looser bowel movements)
- Unexplained tiredness
- Unexplained weight loss
- A pain or lump in your abdomen (stomach)
The symptoms outlined above are often caused by something less serious and don’t usually mean it’s cancer. However, finding cancer early makes it more treatable and a trip to your doctor could save your life. So if in doubt get checked out.
Reduce your risk
Certain lifestyle factors can increase your risk of bowel cancer, such as too much red and processed meat, too much fatty food, too much alcohol, obesity and not enough physical activity.
The following can help to reduce your risk:
- Eat plenty of fibre such as oats, pulses (peas, beans and lentils), fruit and vegetables, cereals, wholegrain bread, wholemeal pasta and brown rice. Also drink plenty of water.
- Cut down on processed meats (bacon, ham, sausages)
- Limit red meat (beef, lamb, pork) consumption to 4-5 portions per week. One portion is the size of a pack of cards
- Eat at least five portions of fruit and vegetables every day
- Maintain a healthy body weight
- Be physically active
- If you drink alcohol, limit your intake. Not drinking alcohol is best for cancer prevention
- Take up any invitation to take part in bowel screening
- Don’t start smoking, or stop if you do (for help to stop smoking visit www.want2stop.info)
For more information on 12 ways to reduce your cancer risk click here.
The bowel screening programme
 In Northern Ireland anyone aged 60 – 74 who is registered with a doctor’s surgery will be invited to take part in the bowel screening programme. This test is offered every two years.
In Northern Ireland anyone aged 60 – 74 who is registered with a doctor’s surgery will be invited to take part in the bowel screening programme. This test is offered every two years.
The screening programme involves a simple testing kit that is sent out to your home to do yourself and return by post. The test is to identify any blood hidden in your bowel movement. If blood is found in the sample, further testing will be offered. Blood in a sample does not necessarily mean cancer.
Make sure you are registered at your doctor’s surgery so that when you reach the target age group you will get an invitation to take part in screening. It is really important to take part in the bowel screening programme when it is offered – early detection means more successful treatment that can save your life.
Download our information leaflet on bowel cancer here.
Find out how to take the test in different languages here.
If you have any concerns about cancer you can talk to one of our specialist nurses on the Cancer Focus NI free information and support NurseLine on 0800 783 3339 (Monday – Friday, 9am – 1pm). You can also email us on nurseline@cancerfocusni.org.